Post-Covid Vaccine Hesitancy in Nigeria
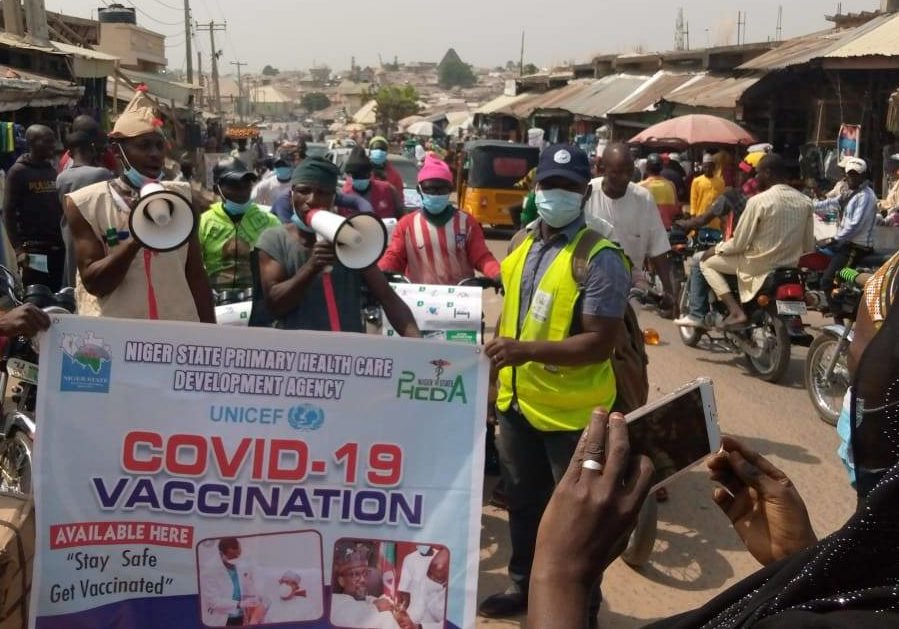

Pictured above: Groups in Nigeria educating the community on the effects and preventative measures of Covid-19.
Pictured to the right: Training for town announcers on key messages to be disseminated during immunisation campaigns
Yet, Nigerians recorded a win in August 2020. The fight against Polio would achieve a milestone, and the Africa Regional Certification Commission (ARCC) would declare Nigeria and Africa Polio free.
Since then, CTG staff have been working for our clients braving Covid-19 conditions whilst battling vaccine hesitancy and misinformation.
I had a conversation with a CTG facilitator who has been working on sensitising caregivers and parents on the available vaccines. She addresses the dangers of infectious diseases and presents the science to those who may not have access to Google in the way you and I do.
Sensitising Communities
Meet Abiola Ogundare. Abiola is a CTG facilitator that has worked for 8 years in the field, as a Communication State Facilitator for Polio and Routine Immunisation. Abiola currently works in the Northern part of Nigeria, where she and a team of Volunteer Committee Mobilisers work on campaigns to aid vaccine delivery at the grassroots level.
Abiola spoke about the work she and her team do, sensitising communities about the vaccine delivery activities.
How have you been sensitising communities?
We have a data-based approach to these things. For example, when working with UNICEF they have what we call VCMs, Volunteer Community Mobilisers. They collect data on which infectious diseases may be a problem in a certain community, as well as which houses or areas are more resistant to immunising children.
There is a team that reviews this data every month to track progress. Armed with that data, we know what conversation we are having with who. Typically, though we tend to focus on infectious diseases like Measles, Meningitis, Polio, and Hepatitis.
What is a “blocker” when trying to sensitise people on the benefit of vaccines?
One of the things that have proven to be an obstacle is that people in these grassroot areas tend to be “seasonal people” – they come and go based on the seasons. For instance, it’s the harvest season and you’ve built a rapport with a family; just when you feel close to a conclusion, the family moves with its harvest. In this sort of case, the fishing season starts and so you have to start the messaging anew, instead of a continuation.
It can be quite disruptive if you don’t have a means of communicating continuously with the caregivers.
What are your concerns when it comes to communication for vaccine compliance?
While I have been stationed in the Northern part of Nigeria, my team and I have tried to sensitise the communities on the prevention of diseases like Measles and polio. I think getting the community to understand that these diseases are preventable through vaccination is a concept that is proving difficult to grasp or accept.
There are also cultural implications in the various geopolitical zones. Sometimes, the caregiver of the child may not be the decision maker over the care received by the child. These instances show that there are sometimes multiple hurdles to overcome.
From talking to Abiola, it seems that the semi-nomadic lifestyle of the communities that she works with significantly affects the ability to ‘follow-through’ on the sensitisation. The social and psychosocial factors that the caregivers live through may be the very thing that rules their entire support system.
Lifestyle and culture of the rural Nigerian may also give legitimacy to why these communities sooner turn to traditional medicine. After all, a few herbs from a trusted community member may be more accessible than a health facility several miles away. This eliminates having to talk to strangers that are typically not from your community.

